Malawi’s ban on dual practice divides health sector
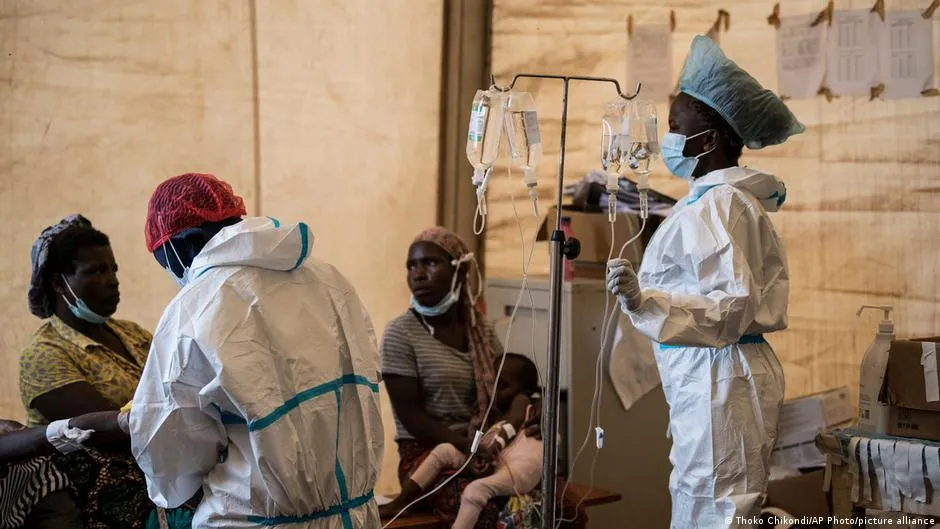
Malawi’s Ban on Dual Practice Sparks Debate
Malawi’s government has enacted a restriction on dual practice, preventing public health professionals from holding private medical roles. While officials claim the policy addresses corruption, many within the medical field argue it could worsen existing staffing shortages.
Directive Targets Corruption in Public Health System
Last month, the Malawian administration imposed a sweeping ban on dual practice, banning public-sector doctors and nurses from working in private clinics, hospitals, pharmacies, or diagnostic centers while employed by the state. The policy also requires any public health worker who owns or partially owns a private facility to divest within 30 days, or risk dismissal and legal consequences.
The measure was prompted by a report from Nyasa Times, which exposed a widespread corruption network in multiple public hospitals. Patients were routinely forced to pay illicit fees for services meant to be free, with security guards, clerks, nurses, and clinicians participating in coordinated bribery schemes. Those who paid could bypass queues, while others waited for days without care.
The investigation revealed how access to treatment had effectively become a cash-based privilege, leaving poor patients without essential services. President Peter Mutharika defended the ban, stating it aims to combat long-standing abuses. He cited cases where staff demanded informal payments, redirected patients to private facilities, and even diverted medicines for resale in their own pharmacies.
Controversy Over Financial Pressures and Innovation
Public-sector wages remain low, prompting many doctors and nurses to rely on private work to meet basic needs. Critics warn the directive could push professionals to abandon public service, exacerbating a severe staffing crisis. Maziko Matemba, head of the Health and Rights Education Program, called the policy “illegal” and said it violates human rights.
“The directive has no basis. It is illegal and an infringement of human rights,” Matemba told DW.
Additionally, specialists fear the rule might stifle medical innovation. “Ownership of private clinics is vital for improving health services,” Matemba noted. “Without it, the medical community may lose momentum in advancing care.”
Legal challenges are already being prepared by the Society of Medical Doctors in Malawi. Solomon Chomba, a key figure in the Human Resource for Health Coalition, called the approach “wrong,” emphasizing its impact on economic rights. He warned that many workers may resign to avoid closing their private practices.
“The policy could push critical expertise out of the public sector,” said Dr. Victor Mithi, president of the Society of Medical Doctors.
Supporters See Long-Term Benefits
Proponents of the ban argue it is a necessary step to restore public trust and ensure equitable access to healthcare. The Malawi Health Equity Network hailed the measure as a “long-overdue intervention” to combat illegal fees and coercion. Some residents echoed this sentiment, noting that public hospitals often lack medication, forcing patients to seek help from privately owned pharmacies.
“The directive is quite okay because here in Malawi we’ve seen that sometimes you go to a public hospital and there is no medication,” one resident remarked.
DW’s report from Lilongwe highlighted that investigations confirmed many of these private pharmacies are run by the same health workers who serve in public roles. Analysts acknowledge that dual practice is just one symptom of deeper systemic issues, including inadequate oversight and chronic drug shortages.
